The Internet of Things (IoT) in healthcare has become a focus for many healthcare businesses. From centralized device network visibility to predictive asset maintenance and remote care, connected IoT-powered solutions expand the reach and scale of what's possible in modern healthcare. While the benefits of making real-time data available in healthcare platforms are no longer in question, the smooth integration of this data into already complex architectures is.
Clinical environments impose strict requirements around reliability, security, data governance, and interoperability with existing systems. Without disciplined architecture and healthcare-specific engineering, IoT initiatives often stall at the pilot stage or introduce new risks rather than reduce them. This is where a deep understanding of the tech integration, regulations, and best practices of software development for the healthcare industry can help.
This article provides insights for CTOs, senior architects, and digital transformation leaders on how IoT technologies can be used in healthcare software development.
The guide answers the following questions:
- What is IoT in healthcare, and why is it necessary to understand the difference from Internet of Medical Things (IoMT)?
- How does IoT in healthcare work in real clinical environments?
- How is IoT used in healthcare?
- What is the impact of IoT in healthcare?
- What are the most common IoT use cases in healthcare today?
- What are the benefits of IoT in healthcare for patients, clinicians, and healthcare operations?
- What challenges and risks do healthcare organizations face when implementing IoT systems?
- How do security, privacy, and compliance requirements affect healthcare IoT design?
- How can IoT systems be integrated with existing healthcare and clinical systems?
- What does it take to implement IoT in healthcare safely and at scale?
Let's see what you need to know about IoT in the healthcare industry in 2026.
What is IoT in healthcare?
IoT in healthcare means the use of connected physical devices such as medical equipment, sensors, wearables, and infrastructure assets. They collect data, transmit it over secure networks, and process it through edge or cloud systems to support clinical care, operations, and decision-making across healthcare environments.
The impact of IoT in healthcare is immense. The technology allows de-siloing healthcare systems and devices that collect healthcare data. As a result, it expands healthcare providers' capabilities and patient care access and treatment, including for those residing in remote, underpopulated areas.
IoT in healthcare vs IoMT: understanding the distinction
These terms are often used interchangeably, especially in high-level discussions about connected care.
IoT in healthcare is a broad term that covers all connected devices and systems used across healthcare environments. This includes not only medical devices but also operational and infrastructure assets, such as asset-tracking tags, environmental sensors, smart beds, building systems, and logistics monitoring solutions. These systems support both clinical and non-clinical workflows and often follow enterprise IoT architecture patterns.
The Internet of Medical Things refers to the subset of IoT devices specifically designed for healthcare applications that are subject to regulatory oversight, such as FDA clearance or CE marking. These devices are typically used for monitoring, diagnostics, and treatment, and must adhere to strict data integrity, validation, and security standards. Examples include patient monitoring devices, infusion pumps, connected imaging equipment, and wearable medical sensors. IoMT systems introduce stricter requirements around validation, data integrity, security controls, and lifecycle management.
While both describe ecosystems of connected devices that generate and exchange health-related data, the difference isn't just in the name. The distinction matters because it directly affects architecture and governance.
IoT systems used for operational efficiency may tolerate different update cycles, data handling models, and risk profiles than IoMT systems tied to patient safety and clinical decisions. Most IoT-based programs span both domains, combining regulated medical devices with non-regulated infrastructure and operational systems. Designing for this mixed environment requires a clear understanding of where regulatory boundaries apply and how they influence system design, integration, and compliance.
Clarity around device types and regulatory scope is not optional. It determines how systems are designed, secured, and governed. With that foundation in place, it is easier to examine how IoT systems are structured and how data flows through real-world clinical settings.
How IoT in healthcare works
IoT in the healthcare industry is a system that connects physical devices to clinical and operational workflows under strict constraints around safety, reliability, and compliance. Understanding how this system is structured is critical for designing solutions that work beyond pilot deployments.
A typical IoT system for healthcare use is built across several layers, each with distinct responsibilities and constraints. Here's an IoT architecture example.
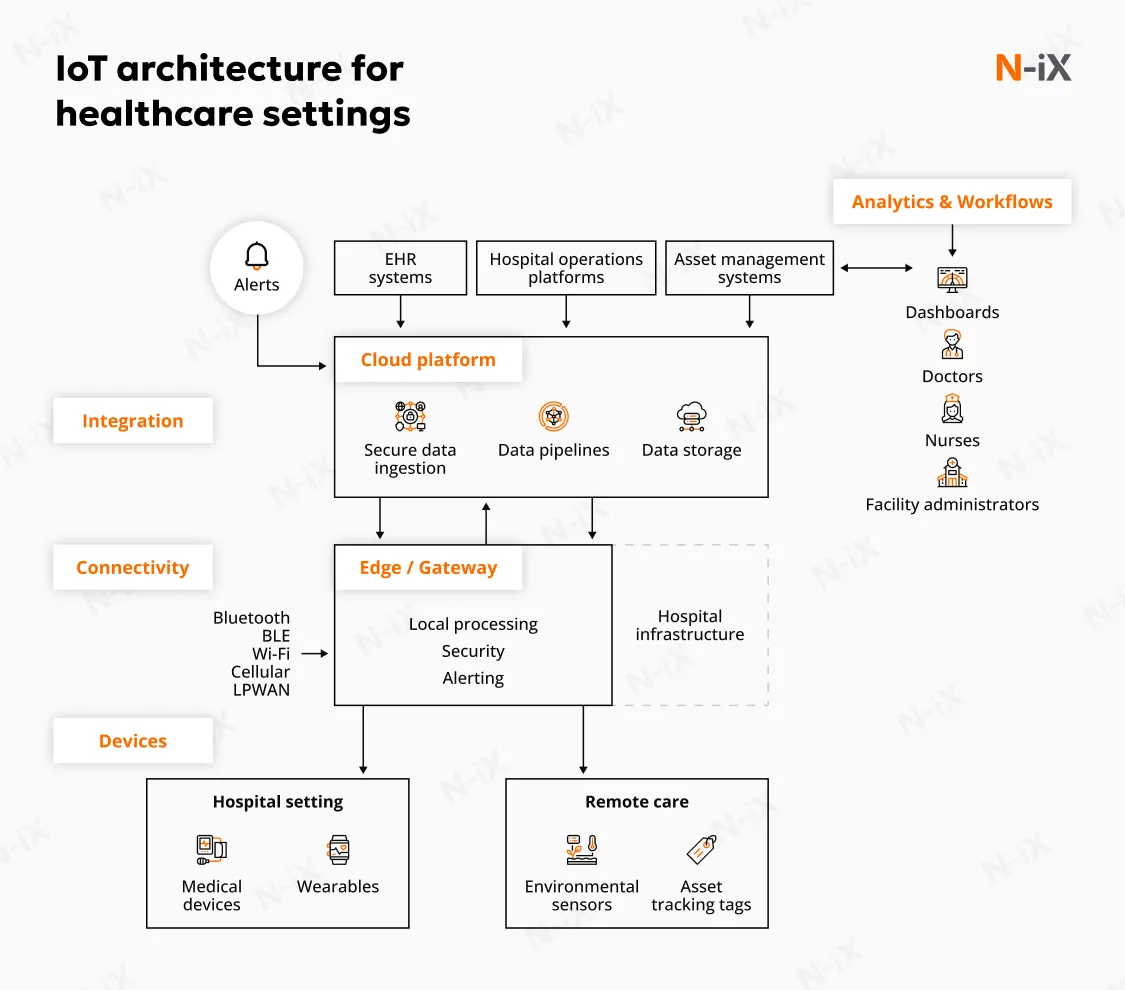
Medical and non-medical IoT devices
Healthcare IoT environments include a mix of regulated and non-regulated devices, such as:
- Patient monitoring devices and medical equipment;
- IoT wearables in healthcare and remote monitoring sensors;
- Environmental sensors (temperature, humidity, air quality);
- Asset tracking tags and smart infrastructure components.
Device selection is influenced by accuracy requirements, battery life, certification status, and how the device fits into clinical workflows.
Connectivity and communication
Devices communicate using different network technologies, depending on clinical and operational needs:
- Bluetooth Low Energy for short-range, low-power communication;
- Wi-Fi for higher bandwidth within facilities;
- Cellular connectivity for mobile or remote use cases;
- LPWAN technologies for low-data, long-life devices.
The choice of IoT connectivity in healthcare directly affects latency, reliability, and power consumption, all of which are critical in industry settings.
Edge processing and gateways
Edge gateways sit between devices and cloud platforms. They typically handle:
- Device aggregation and protocol translation;
- Local data processing and filtering;
- Security enforcement and device authentication;
- Local alerting when immediate action is required.
Edge processing is especially important in healthcare environments where network disruptions are possible. It's required when:
- Immediate alerts or actions are needed;
- Connectivity cannot be guaranteed;
- Clinical safety depends on local decision-making;
- Systems must remain operational during outages.
Cloud ingestion and data pipelines
Cloud platforms are used to ingest, store, and process IoT data at scale. In healthcare, cloud pipelines must support:
- Secure data transmission and storage;
- Data normalization across device types;
- Scalability across patients, facilities, and regions;
- Auditability and traceability for compliance.
Cloud processing makes sense when aggregating data across patients or facilities, performing long-term trend analysis, supporting predictive analytics and optimization, and scaling analytics across large device fleets. Most Internet of Things solutions in healthcare combine edge and cloud processing, using each where it best supports safety, reliability, and scale.
Explore 8 transformative use cases of digital twins in healthcare—get the white paper!


Success!

Integration with clinical and operational systems
IoT data only becomes useful when it is integrated with existing systems, including:
- Electronic health record systems;
- Asset and inventory management platforms;
- Facility management and operations tools.
This integration layer is often one of the most complex parts of healthcare IoT, as it must align real-time device data with patient context and operational processes.
Analytics, alerts, and workflows
At the top of the architecture are analytics and workflows that turn data into action. These may include:
- Real-time alerts for clinicians or operations teams;
- Analytics for trend analysis and optimization;
- Dashboards tailored to different stakeholder roles.
Alerting must be carefully designed to avoid false positives and alert fatigue, which can undermine clinical trust.
Healthcare-specific constraints across all layers
Healthcare-specific constraints shape design decisions across the entire architecture. Most common limitations are associated with:
- Latency: some use cases require near-instant response;
- Reliability: systems must function during outages or degraded connectivity;
- Battery life: especially critical for wearables and remote devices;
- Clinical safety: systems must fail safely and predictably;
- Regulatory boundaries: data handling and processing must align with compliance requirements.
With a clear view of how IoT systems are structured in healthcare and where decisions are made, it becomes easier to estimate the value and benefits these systems deliver across different stakeholders in the organization.
Benefits of IoT in healthcare depending on stakeholders
The value of IoT in healthcare depends on who is using the data and how it is embedded into daily workflows. When designed correctly, IoT systems can change how care is delivered, operations are managed, and risk is controlled across the organization. Here's how IoT helps in healthcare environments to reach the goals of various stakeholders.
Benefits for patients
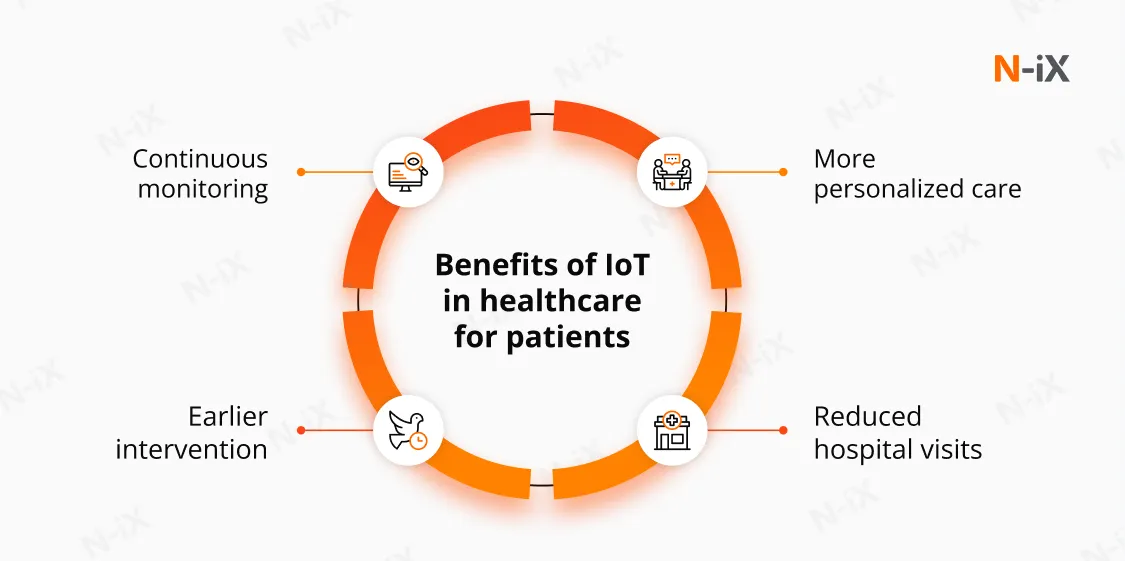
For patients, IoT enables continuous data collection beyond episodic clinical visits.
- Continuous monitoring. Connected devices capture vital signs and health indicators in near real time, providing clinicians with ongoing visibility into a patient’s condition instead of isolated snapshots.
- Earlier intervention. Automated thresholds and alerts surface changes in patient status sooner, allowing care teams to intervene before conditions escalate.
- Reduced hospital visits. Remote monitoring and home-based devices reduce the need for routine in-person checkups, lowering patient burden while preserving clinical oversight.
- More personalized care. Longitudinal data supports individualized treatment adjustments based on real-world patient behavior and trends rather than periodic assessments alone.
These mechanisms help reduce avoidable readmissions, support chronic disease management, and improve continuity of care without increasing clinical workload.
Benefits of IoT in healthcare for clinicians
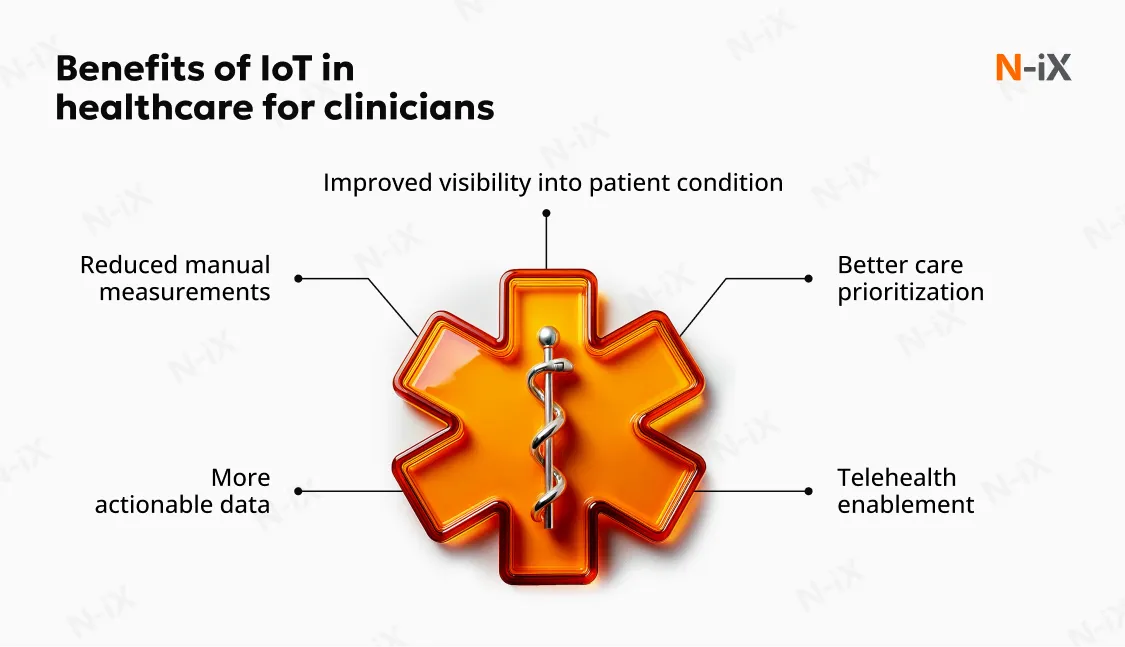
For clinicians, IoT systems are most effective when they simplify decision-making rather than add noise.
- Improved visibility into patient condition. Aggregated device data provides a more complete view of patient conditions across settings, supporting better-informed clinical decisions.
- Reduced manual measurements. Automated data capture replaces repetitive manual tasks, freeing clinical time for patient interaction and higher-value care activities.
- More actionable data. When data is filtered, contextualized, and integrated into clinical systems, clinicians receive insights rather than raw telemetry.
- Better care prioritization. Alerting and dashboards help clinicians focus attention on patients who need intervention most urgently.
- Telehealth enablement. IoT is a core technology for telemedicine software development , enabling providers to expand their offerings and tap into telehealth services. It helps business owners and practitioners to cover more patients and increase revenue.
When IoT data is aligned with clinical workflows, it reduces cognitive load and supports faster, more confident decision-making.
Benefits for healthcare facility administrators

From an operational perspective, IoT improves visibility into assets, facilities, and infrastructure.
- Improved asset utilization. Real-time location and usage data help organizations understand where equipment is, how often it is used, and where bottlenecks occur.
- Reduced equipment loss. Tracking devices and automated inventory updates reduce losses, shrinkage, and time spent searching for critical equipment.
- Predictive maintenance. Device telemetry supports early detection of wear or failure, reducing unplanned downtime and extending equipment lifespan.
- More efficient facility management. Environmental sensors provide data to optimize space usage, energy consumption, and compliance with storage or safety requirements.
These capabilities translate into lower operational costs, higher equipment availability, and more reliable service delivery.
Healthcare IoT benefits for IT and security teams

For IT and security teams, IoT introduces new complexity but also new opportunities for control.
- Centralized device network visibility. A unified view of connected devices makes it easier to manage inventory, firmware versions, and system health.
- Policy-driven access control. Device and user identities can be managed consistently, reducing unauthorized access and configuration drift.
- Improved auditability. Centralized logging and monitoring support compliance reporting and incident investigation.
- Reduced security risk. Proactive monitoring and standardized controls help detect anomalies and enforce security baselines across device fleets.
When IoT is engineered with governance in mind, it strengthens the security posture rather than expanding risk.
While these benefits are compelling, they only materialize when IoT systems are applied to the right problems and use cases. The next section explores the most common and impactful IoT use cases in healthcare and how they are implemented in practice.
Key use cases of IoT in healthcare
IoT in healthcare delivers value only when it is applied to clearly defined clinical or operational problems. Below is how IoT can be used in healthcare with cases, structured consistently to show what problem is solved, how data is used, and what it takes to make each scenario work in real healthcare environments.

Remote patient monitoring (RPM)
Remote patient monitoring (RPM) extends care by tracking vital health data, such as heart rate, glucose levels, and oxygen saturation, using devices like wearable ECG monitors and continuous glucose sensors. It’s widely used among patients with chronic conditions, those with post-acute needs, or those in recovery programs in home or outpatient settings. According to Verizon's 2025 IoT Market Insights Report, 56% of surveyed healthcare businesses use IoT for remote patient monitoring [1].
What data is collected: Vital signs such as heart rate, blood pressure, oxygen saturation, glucose levels, activity data, and symptom inputs.
Where data is processed: Initial validation and threshold checks often happen at the edge or gateway. Aggregation, trend analysis, and reporting are typically handled in the cloud.
Who acts on the data: Clinicians, care coordinators, and remote monitoring teams.
In practice, RPM platforms must balance clinical safety with usability. This is reflected in projects where connected monitoring data is tightly integrated with digital care platforms, enabling clinicians to act on insights rather than raw telemetry.
Wearable healthcare devices
Wearable healthcare devices enable continuous, non-intrusive patient monitoring in everyday settings. Unlike episodic clinical measurements, wearables provide longitudinal health data that supports earlier detection of changes, trend-based diagnosis, and more informed clinical decision-making.
What data is collected: Modern healthcare wearables capture a range of physiological and behavioral metrics, including:
- Heart rate and heart rate variability
- Blood pressure and oxygen saturation
- Glucose levels via continuous monitoring devices
- Activity, sleep patterns, and movement data
Collected over time, this data provides context that single-point measurements cannot capture.
Where data is processed: Basic signal validation and noise filtering typically occur on the device or at the edge. Cloud platforms aggregate longitudinal data, correlate it with other clinical inputs, and support analysis across populations or time periods.
Who acts on the data: Clinicians, chronic care teams, and diagnostic specialists, often supported by care coordinators and remote monitoring staff.
Wearables deliver the most value when they are treated as clinical data sources rather than consumer gadgets. Their strength lies in longitudinal insight, where trends and deviations over time support more accurate diagnosis and proactive care, provided the data is properly validated and contextualized.
Disease-specific monitoring
Disease-specific monitoring applies IoT to track patients with well-defined chronic or progressive conditions where continuous, condition-tailored data is critical. Unlike generic RPM, these systems focus on disease-relevant indicators to support earlier intervention, symptom management, and treatment adjustments for conditions such as diabetes, cardiac disorders, and neurological diseases.
What data is collected: The data collected varies by condition and is tailored to clinically meaningful signals, for example:
- Diabetes: continuous glucose levels, insulin dosing events, activity patterns
- Cardiac conditions: heart rate variability, ECG signals, blood pressure, arrhythmia indicators
- Neurological conditions (e.g., Parkinson’s): movement patterns, tremor frequency, gait stability, medication timing and response
In many cases, this data is complemented by patient-reported symptoms to provide clinical context.
Where data is processed: Time-sensitive validation and threshold detection typically occur at the device or edge level to ensure rapid response. Cloud platforms aggregate longitudinal data, correlate trends over time, and support condition-specific analytics and reporting.
Who acts on the data: Specialist clinicians, chronic care teams, and care coordinators who manage disease-specific treatment plans and interventions.
In practice, disease-specific monitoring systems succeed when IoT data is tightly aligned with clinical protocols for each condition. Rather than relying on generic alerts, these platforms translate raw device data into condition-aware insights that support targeted decision-making and long-term disease management.
Connected inpatient monitoring
Continuous monitoring inside hospitals improves patient safety by providing real-time visibility into patient status between scheduled checks. This is especially useful for hospitals at home (H@H), palliative care centers, and end-of-life support.
What data is collected: Vital signs, movement data, device status, and alarm events from bedside equipment.
Where data is processed: Edge processing is critical for real-time alerts. Cloud platforms support aggregation, reporting, and retrospective analysis.
Who acts on the data: Nurses, physicians, and rapid response teams.
Connected inpatient monitoring systems must be designed with clinical workflows in mind, ensuring alerts are meaningful and actionable.
Our case study portfolio also includes a few examples of IoT in healthcare. At N-iX, we supported WEINMANN Emergency in enhancing their portable defibrillator, MEDUCORE Standard ², by integrating advanced telemetry and Bluetooth printer functionalities. Our team developed secure communication protocols and improved device connectivity. It allows for ECG data to be instantly shared with doctors via email or fax, facilitating faster medical response and remote medical assistance.
Medication adherence systems
Medication non-adherence is a major contributor to poor outcomes, especially for chronic conditions and post-discharge care.
What data is collected: Medication dispensing events, timestamps, patient confirmations, and adherence patterns.
Where data is processed: Edge devices capture events locally, while cloud systems analyze adherence trends and trigger reminders or escalations.
Who acts on the data: Patients, care coordinators, and clinicians.
Effective medication adherence solutions focus as much on user experience as on technical accuracy, ensuring devices are easy to use and data flows support timely interventions.
Hospital asset tracking
Hospitals often struggle with locating critical equipment, leading to delays, excess inventory, and unnecessary purchases.
What data is collected: Location data, movement history, usage duration, and device status.
Where data is processed: Edge gateways handle real-time location signals, while cloud platforms support analytics and utilization reporting.
Who acts on the data: Operations teams, biomedical engineering, and logistics staff.
Asset tracking initiatives are most effective when they are integrated into operational workflows rather than treated as standalone tools.
Explore further: IoT in asset management: Making use of connected technologies
Cold chain monitoring (pharma and labs)
Temperature-sensitive medications, vaccines, and lab samples require strict environmental control during storage and transport.
What data is collected: Temperature, humidity, location, and time-based exposure data.
Where data is processed: Edge processing validates thresholds locally, while cloud systems provide audit trails and compliance reporting.
Who acts on the data: Pharmacy teams, lab managers, and compliance officers.
Cold chain solutions must prioritize reliability and traceability to support regulatory compliance.
Predictive maintenance of medical equipment
Unplanned downtime of critical medical equipment disrupts care delivery and increases operational risk.
What data is collected: Equipment usage metrics, performance indicators, error codes, and environmental conditions.
Where data is processed: Edge systems collect and preprocess telemetry, while cloud analytics identify degradation patterns.
Who acts on the data: Biomedical engineering and maintenance teams.
Predictive maintenance programs benefit from close alignment between IoT engineering and equipment domain expertise, as seen in embedded development projects for healthcare device manufacturers.
As part of our collaboration with WEINMANN Emergency to improve their MEDUCORE Standard² defibrillator, we had to ensure the device met strict healthcare regulations and supported predictive maintenance. By seamlessly integrating with the client’s team and applying Agile methodologies, we helped streamline development and enhance the product’s overall functionality.
Environmental monitoring and infection control
Environmental conditions and staff hygiene practices directly affect infection risk, patient safety, and regulatory compliance. IoT supports infection control by continuously monitoring clinical environments and reinforcing hygiene protocols, reducing reliance on manual checks and retrospective audits.
What data is collected:
- Environmental data (temperature, humidity, air quality, and room conditions, etc.)
- Hand hygiene events, including sanitizer dispenser usage, staff entry and exit patterns, and proximity-based interactions.
- Time and location data to correlate hygiene actions with specific rooms or care activities.
Where data is processed: Immediate validation and reminders are handled at the edge to ensure real-time feedback. Cloud platforms aggregate data across facilities, support trend analysis, and provide compliance reporting over time.
Who acts on the data: Infection control teams, facility management, compliance officers, and clinical leadership that are responsible for safety protocols.
IoT-enabled infection control systems are most effective when environmental monitoring is combined with hand hygiene compliance tracking. Rather than relying solely on scheduled audits, these systems provide real-time reminders, objective compliance data, and actionable insights. When integrated into facility operations and safety programs, they help reinforce consistent hygiene behavior and support measurable reductions in infection risk.
N-iX has a recent IoT in healthcare case study where we’ve helped healthcare businesses adopt IoT for environmental monitoring. Our client, a company specializing in the development of air decontamination devices, needed to improve the performance and usability of its system.
We developed custom firmware and upgraded the hardware, ensuring stable and efficient operation. Additionally, we created a cross-platform mobile app for remote system management. As a result, we ensured stable operation of the decontamination system, enhanced its reliability, and improved usability and user experience.
Learn more about healthcare mobile app development from our comprehensive guide
Ingestible and implantable IoT devices
Ingestible and implantable IoT devices enable monitoring and intervention when external sensors are insufficient. These technologies support condition-specific diagnostics, therapy adherence, and precision procedures by collecting data directly from within the body or by augmenting clinical procedures with connected systems.
What data is collected: The data collected depends on the device and application, including:
- Physiological data from ingestible sensors, such as temperature, pH levels, or medication ingestion confirmation
- Intraocular pressure and biochemical indicators from smart contact lenses
- Device telemetry and procedural data from implantable or robot-assisted surgical systems
Where data is processed: Initial data capture and validation occur within the device itself, with secure transmission to nearby receivers or gateways. Cloud platforms handle aggregation, longitudinal analysis, and integration with clinical systems where appropriate.
Who acts on the data: Specialist clinicians, surgeons, and care teams responsible for diagnostics, treatment planning, or procedural execution.
Ingestible and implantable IoT systems demand a higher level of engineering rigor than most external monitoring solutions. Success depends on reliable embedded software, secure communication, and careful alignment with regulatory and clinical requirements. When IoT implementation in healthcare is done correctly, these technologies extend IoT capabilities into healthcare areas where traditional sensing approaches are not feasible.
Staff safety and workflow optimization
Healthcare staff face safety risks and workflow inefficiencies, particularly in high-pressure environments.
What data is collected: Location data, movement patterns, panic alerts, and workload indicators.
Where data is processed: Edge processing supports immediate alerts, while cloud systems analyze workflow patterns.
Who acts on the data: Operations leaders, security teams, and clinical managers.
Successful implementations focus on transparency and clear value for frontline teams.
Insurance-driven healthcare IoT
Healthcare IoT enables insurers to move from retrospective assessment to continuous, data-informed decision-making. By incorporating IoT-generated health and behavior data, insurers can improve risk assessment, streamline claims processing, and detect anomalies earlier. At the same time, healthcare providers benefit from aligned incentives around prevention and adherence.
What data is collected:
- Patient health metrics from wearables and remote monitoring devices, such as activity levels, vital signs, and condition-specific indicators
- Usage and adherence data from connected medical devices
- Environmental and event data that provides context for claims or incidents
This data is usually collected with explicit consent and governed by strict privacy and compliance requirements.
Where data is processed: Initial validation and aggregation may occur at the edge or within the IoT platforms. Cloud systems support longitudinal analysis, correlation with policy and claims data, and integration with insurer analytics and reporting systems.
Who acts on the data: Insurance analytics teams, underwriting specialists, claims processors, and fraud detection units, often in coordination with healthcare providers and care management teams.
In practice, insurance-driven healthcare initiatives are most effective when they focus on transparency and value creation for all parties. Rather than using IoT data solely for risk control, leading programs align incentives by rewarding preventive behavior, supporting chronic condition management, and improving coordination between insurers and healthcare providers.
Robotic surgery and connected surgical systems
Robotic surgery systems extend surgical precision and consistency in complex procedures where human dexterity alone reaches its limits. By combining connected surgical instruments, real-time sensing, and data-driven control, these systems support minimally invasive procedures, reduce surgeons' physical strain, and improve procedural repeatability across operating rooms.
What data is collected: Connected surgical systems generate and process multiple data streams, including:
- Instrument position, force, and movement data
- High-resolution imaging and video feeds
- System telemetry, calibration data, and error signals
- Procedural timing and workflow data
This data enables precise control, monitoring, and post-procedure analysis.
Where data is processed: Time-critical control and feedback loops are handled locally within the robotic system and edge infrastructure to ensure safety and low latency. Cloud platforms are used selectively for procedural analysis, performance benchmarking, training insights, and system optimization.
Who acts on the data: Surgeons, operating room teams, biomedical engineers, and surgical system manufacturers responsible for performance, maintenance, and procedural quality.
Connected surgical systems rely on IoT principles to function safely and effectively. Advances in high-speed, low-latency connectivity, including private networks and 5G, are expanding the potential for remote assistance and specialist collaboration, particularly in regions with limited access to expert surgical care. When designed with safety and governance in mind, IoT-enabled robotic surgery systems enhance surgical capabilities while maintaining strict clinical control.
Explore robotics in healthcare: Applications and benefits
Across these use cases, one pattern remains consistent: IoT delivers results only when technical design, clinical context, and operational workflows are aligned. Case studies involving digital healthcare platforms, emergency medical equipment, and regulated embedded systems demonstrate that real-world healthcare IoT requires disciplined architecture, deep domain understanding, and close collaboration with clinical stakeholders.
Challenges of IoT in healthcare
IoT initiatives in healthcare often struggle not because the technology is immature, but because clinical environments impose constraints that are easy to underestimate. Security, interoperability, and operational realities intersect in ways that require disciplined engineering and healthcare-specific experience. Below are the most common challenges, why they occur, and how N-iX addresses them in practice.

Security, privacy, and compliance
IoT systems in healthcare environments are uniquely exposed. They combine a rapidly growing number of connected devices with long device lifecycles, legacy clinical systems, and multiple third-party dependencies. Each device and integration point expands the attack surface, while regulatory requirements limit how quickly systems can be changed or patched. Unlike consumer IoT, IoT vulnerabilities in healthcare here may directly affect patient safety and data protection.
How N-iX solves it: N-iX approaches healthcare IoT with a compliance-by-design mindset focused on engineering controls rather than policy statements. Our teams design systems that enforce data minimization by default, apply encryption in transit and at rest, and use strong device identity and authentication mechanisms. Role-based access, centralized audit logging, traceability, secure booting mechanisms and device identity management are built into the architecture from the start. Secure firmware update mechanisms and controlled lifecycle management ensure devices remain maintainable in regulated environments without disrupting clinical operations.
Interoperability and integration with clinical systems
IoT data has limited value if it remains isolated from clinical and operational systems. Integrating device data into EMRs, EHRs, and care workflows is difficult due to heterogeneous device protocols, inconsistent data models, patient identity mapping, and consent requirements. Poor integration often leads to alert fatigue, duplicated workflows, or data that clinicians do not trust or use.
How N-iX solves it: N-iX focuses on interoperability patterns that align IoT data with clinical context. This includes normalizing device telemetry into clinically meaningful events, mapping data reliably to patient identities, and integrating alerts into existing clinical systems instead of creating parallel tools. We design alerting logic to prioritize relevance and reduce noise, and we work with legacy systems through well-defined integration layers rather than brittle point-to-point connections. This approach ensures that IoT data supports decision-making rather than overwhelming care teams.
Explore further: EMR & EHR software development: All you need to know
Integration of AI and IoT
AI is already widely used in healthcare for image analysis, clinical decision support, risk stratification, and operational optimization, where it relies on historical datasets from EHRs, imaging systems, and claims data. And it can do much more with continuous, real-world patient and device data from IoT devices. The combination of AI and IoT in healthcare is highly desirable for improving healthcare services. It's also challenging.
AI depends on data that is not only large in volume but also consistent, reliable, and clinically meaningful. In real healthcare environments, IoT data is often noisy, incomplete, delayed, or generated under varying conditions. Without proper validation, context, and governance, AI systems trained on raw IoT telemetry can produce misleading insights, biased predictions, or recommendations that clinicians do not trust. The stakes are high: flawed AI outputs can affect clinical decisions, introduce patient safety risks, and undermine regulatory compliance. At the same time, operationally immature AIoT applications can increase system complexity, inflate costs, and create opaque decision logic that is difficult to audit or explain.
How N-iX solves it: N-iX approaches AI and IoT integration as a governed, end-to-end engineering challenge rather than a bolt-on analytics layer. We design IoT architectures that can prepare data for AI from the start, applying validation, normalization, and contextual enrichment before data reaches analytics pipelines. Our teams align AI outputs with clinical workflows, ensuring models generate explainable, role-specific decision-support insights rather than opaque, black-box predictions. We also embed monitoring, versioning, and auditability into AI pipelines to support regulatory requirements and long-term operability. By tightly coupling IoT engineering, data architecture, and AI expertise, N-iX helps healthcare organizations deploy AI-powered IoT systems that are trustworthy, transparent, and safe to use in real clinical settings.
Implementation challenges in real healthcare environments
Many applications of IoT in healthcare fail during rollout or scaling. Common issues include unreliable hospital networks, fragmented device provisioning processes, inconsistent data quality, and a lack of alignment with clinical workflows. While pilots may succeed under controlled conditions, they may break down when exposed to real-world variability, operational load, and organizational change.
How N-iX solves it: N-iX designs IoT systems for healthcare use with production conditions in mind from the outset. Our teams account for network variability through resilient architectures and edge processing. We implement structured device provisioning and lifecycle management to support scale. Data quality controls and validation mechanisms reduce false positives before data reaches clinicians. Most importantly, we work closely with stakeholders to align technical design with clinical and operational workflows, addressing adoption risks early rather than after deployment.
These challenges explain why effective performance of IoT in healthcare requires more than technical integration. It demands an understanding of clinical risk, regulatory boundaries, and operational reality. Addressing them systematically is what turns IoT from a pilot initiative into a reliable part of healthcare delivery.
How to implement IoT in healthcare: A practical roadmap
Successful projects of IoT in healthcare follow a disciplined, phased approach. The goal is not rapid deployment, but controlled implementation that balances innovation with clinical safety, regulatory compliance, and operational stability.
Discovery and clinical workflow analysis
Implementation starts with understanding how care is delivered today. This phase focuses on identifying where IoT data can support clinical or operational decisions, who will act on that data, and how it fits into existing workflows. Early clarity here prevents solutions that generate data without clear ownership or impact.
Architecture and security design
Once use cases are defined, architectural decisions set the system's long-term trajectory. Key tradeoffs include edge versus cloud processing, connectivity options, and integration patterns with clinical systems. Security and compliance controls must be designed into the architecture from the outset, as retrofitting them later is costly and disruptive.
Pilot with success criteria
Pilots should be designed as controlled experiments, not proofs of concept. Clear success metrics, defined user groups, and operational readiness criteria help validate both technical performance and clinical usability. This phase is where assumptions are tested against real-world conditions.
Validation and risk assessment
Before scaling, systems must be validated against reliability, safety, and compliance requirements. This includes testing under degraded network conditions, verifying alert behavior, and confirming data integrity. Risk assessment at this stage reduces surprises during broader rollout.
Production rollout
Scaling introduces new challenges, from device provisioning to support processes. A structured rollout plan ensures consistent configuration, monitoring, and governance across facilities and device fleets.
Ongoing operations and optimization
IoT-based healthcare systems require continuous oversight. Monitoring, patch management, performance tuning, and periodic review of clinical workflows help ensure the system remains effective as requirements evolve.
When approached systematically, this roadmap turns IoT from a series of disconnected initiatives into a sustainable capability. That's where an experienced IoT software development company like N-iX can help.
Explore the top 15 healthcare IT consulting companies for your next project
Selecting technologies and partners for developing IoT projects in healthcare
Early technology choices in a healthcare IoT initiative have long-term consequences. Devices, platforms, and partners that work well in generic IoT environments often fall short in clinical settings, where reliability, safety, and compliance are non-negotiable.
How to evaluate core components
When adopting the Internet of Things in healthcare, you need to evaluate core components of the potential IoT solution to fit your specific use case, scenario, and setting. Here are a few examples by component.
- Devices and sensors. Look beyond technical specifications. Evaluate certification status, data accuracy, battery life, update mechanisms, and how devices behave under failure conditions. In healthcare, device lifecycle management and validation matter as much as functionality.
- Connectivity. No single connectivity model fits all use cases. Mobility, latency requirements, power constraints, and environmental conditions should drive selection. Architectures that support multiple connectivity options are more resilient in real clinical environments.
- IoT platforms. They must support secure ingestion, scalable data pipelines, and auditability. Equally important is how well they integrate with existing clinical and operational systems. Platforms that require extensive customization to fit healthcare workflows introduce hidden risk.
- Integration approach. Integration is often the most complex part of healthcare IoT. Prioritize architectures that normalize device data, support patient context mapping, and avoid brittle point-to-point connections with legacy systems.
- Security features. Security should be evaluated as an architectural capability, not a feature checklist. Device identity, access control, monitoring, and update mechanisms must be consistent across the entire system.
Common red flags to watch for:
- “Out-of-the-box” solutions that require minimal configuration
- Platforms that treat compliance as a documentation exercise
- Limited visibility into device lifecycle and update processes
- Integrations that bypass clinical systems rather than work with them
Healthcare IoT is rarely plug-and-play because clinical environments combine regulated devices, legacy systems, and strict operational constraints. Success depends on making informed tradeoffs and selecting technologies that can be governed over time, not just deployed quickly.
Our expertise in providing custom IoT services for healthcare businesses
Healthcare IoT systems succeed or fail at the architectural level. Devices, connectivity, data pipelines, security controls, and clinical integrations must work together under strict regulatory and reliability constraints. N-iX supports healthcare organizations across every layer of the IoT architecture, helping reduce risk and complexity from the outset.
Device and firmware layer
At the foundation are connected medical and non-medical devices that must operate reliably over long lifecycles.
N-iX helps healthcare organizations with:
- Embedded software development for healthcare-grade devices, focusing on stability, deterministic behavior, and maintainability;
- Firmware development covering device control logic, communication stacks, secure boot, and update mechanisms;
- Connected device engineering to integrate sensors, connectivity modules, and hardware platforms into production-ready devices.
This layer is critical in regulated environments, where failures directly affect patient safety and where post-deployment updates must be carefully controlled.
Connectivity and edge layer
Healthcare environments impose constraints on latency, reliability, and network availability that generic IoT architectures often overlook.
N-iX assists with:
- Connectivity design and implementation across BLE, Wi-Fi, cellular, and hybrid models;
- Edge and gateway engineering for local processing, buffering, security enforcement, and resilience during network disruptions;
- Device provisioning and fleet management to support scaling beyond pilot deployments.
This layer ensures that IoT systems continue to function in healthcare settings even under degraded network conditions.
IoT platform and cloud data layer
At scale, healthcare IoT systems depend on robust cloud architectures that can ingest, process, and govern sensitive data.
We have over 400 cloud and over 200 data experts to help you with:
- IoT cloud solutions development, including cloud ingestion pipelines, data normalization, scalable storage, and cloud security;
- IoT platform integration tailored to healthcare requirements for auditability, traceability, and compliance;
- Analytics and data processing to support both real-time insights and long-term population-level analysis.
Architectural decisions at this layer determine whether IoT systems can grow without introducing operational or compliance risk.
Learn more about the best approaches to data governance in healthcare
Application and user experience layer
IoT data must be usable by clinicians, patients, and operational teams to create value.
With N-iX, you can expect custom services, including:
- Wearable and mobile application development that connects patient-facing devices to backend IoT systems;
- UI/UX design for healthcare platforms, ensuring data is presented clearly and supports clinical decision-making;
- IoT data visualization solutions with role-based dashboards and alerts aligned with real workflows to avoid alert fatigue.
This layer bridges technical systems and human interaction, where adoption often succeeds or fails.
Integration and interoperability layer
IoT in healthcare rarely operates in isolation or for a limited number of devices. Integrating IoT applications in healthcare with other systems requires knowledge of the technical requirements and regulations specific to connected healthcare solutions (HIPAA, HL7, FIHR, etc.).
N-iX specializes in:
- Integration with EHRs and clinical systems, mapping device data to patient context;
- Ensuring interoperability with legacy healthcare platforms, using resilient integration patterns;
- Workflow-aligned data delivery, embedding IoT insights into existing clinical and operational processes.
This layer ensures IoT enhances existing systems rather than competing with them.
Security, compliance, and governance layer
Security and compliance are paramount at every architectural layer. According to IBM and Red Hat’s 2025 Threat Intelligence Index, the healthcare industry accounted for 5% of security incidents in 2024 [3]. Given that healthcare is among the top-ten often-targeted domains by cyberattackers, security practices, compliance, and governance should be incorporated into the design from the start.
For IoT-powered healthcare solutions, N-iX offers:
- IoT security services covering device identity, secure communication, access control, monitoring, and incident readiness;
- Compliance-by-design engineering, embedding auditability and traceability into system architecture;
- Lifecycle governance, ensuring systems remain secure and compliant as devices, software, and regulations evolve.
By working across all layers of the IoT architecture, N-iX helps healthcare organizations move from fragmented initiatives to cohesive, production-ready IoT systems. This end-to-end approach reduces integration risk and creates systems that can be trusted in real clinical environments.
Final thoughts
IoT in healthcare is a foundation for delivering connected care, managing healthcare facilities with lesser risks and more convenience, and making use of real-time data. The organizations that succeed are those that approach IoT as a system-level investment, grounded in clinical realities, regulatory discipline, and long-term operability.
For healthcare leaders, the challenge is not understanding the potential of IoT, but turning that potential into production-ready systems that can be trusted at scale. Doing so requires architectural rigor, security-first engineering, and experience navigating regulated environments from device to cloud. With experience in IoT consulting services and development, N-iX is your trusted tech partner.
We work with healthcare organizations to help them design, build, and operate IoT healthcare systems that move beyond pilots and deliver measurable impact in real clinical settings. Let's talk about where IoT adoption can solve your business challenges and create solutions that last.
Sources:
- 2025 IoT Market Insights Report | Verizon Business
- Eseye 2024 State of IoT Adoption | Eseye
- IBM X-Force 2025 Threat Intelligence Index | IBM
- 2025 Tech Trends Report | Future Today Strategy Group (FTSG)
Key takeaways
- IoT in healthcare connects devices for real-time data exchange, improving patient care and operational efficiency by enabling continuous monitoring and faster decision-making.
- Wearable devices and remote monitoring are driving healthcare innovation, allowing clinicians to track vital signs remotely and intervene earlier, reducing hospital visits.
- Data security and compliance are critical in healthcare IoT, ensuring patient data protection and adherence to regulations like HIPAA while maintaining system reliability.
- Integrating IoT with existing clinical systems is key to ensuring real-time data supports clinical workflows and reduces alert fatigue.
- IoT in healthcare offers transformative benefits across various use cases, from predictive maintenance to environmental monitoring, improving both patient outcomes and operational efficiency.
FAQ
What is IoT technology in healthcare?
IoT technology in healthcare refers to the ability of devices to collect and transmit health-related data for further processing to improve patient care, operational efficiency, and decision-making.
What are the examples of IoT devices used in healthcare?
Examples of IoT in healthcare include wearable health trackers, remote patient monitoring devices, connected defibrillators, and smart hospital equipment. These devices enable continuous monitoring of vital signs, improve patient outcomes, and streamline hospital operations through real-time data transmission.
Why is IoT important in healthcare?
IoT is crucial in healthcare because it enables remote patient health monitoring, enabling more proactive care. It also helps optimize hospital operations, reduce costs, and improve decision-making.
What is a key benefit of IoT in healthcare?
A key benefit of IoT in healthcare is the ability to connect healthcare systems and devices to enable real-time data exchange of healthcare information.
What are the challenges of IoT in healthcare?
The main challenges of IoT in healthcare include data privacy, integration with existing clinical systems, and device security. Additionally, the reliability of IoT devices, regulatory compliance, and the management of large volumes of real-time data can complicate implementation.
What are the common areas in which IoT can be used in healthcare?
Common IoT applications in healthcare include remote patient monitoring, disease-specific monitoring, environmental and infection control, and asset tracking in hospitals. IoT also improves medication adherence and enables predictive maintenance of medical equipment to ensure seamless operations.
What is the application of IoT in healthcare?
IoT is applied in healthcare to connect devices like sensors, wearables, and medical equipment, enabling continuous data collection, monitoring, and analysis. Applications include real-time tracking of patient vitals, equipment maintenance, and improving operational workflows within healthcare facilities.
Why does security matter for IoT in healthcare?
Security is critical for IoT in healthcare to protect sensitive patient data from breaches and ensure compliance with regulations like HIPAA, GDPR, and others. Secure communication protocols, encrypted data storage, and device authentication are necessary to maintain patient privacy and prevent unauthorized access to medical systems.
What are the IoT trends in healthcare?
Key IoT trends in healthcare include the rise of wearable health devices for continuous monitoring, the integration of AI and machine learning for predictive analytics, and the use of remote patient monitoring to reduce hospital visits. Additionally, advancements in 5G technology are enabling faster, more reliable data transmission, while edge computing is improving real-time decision-making at the point of care.
What is the future of IoT in healthcare?
The future of IoT in healthcare is focused on enhancing patient care through smarter, more connected devices. We can expect increased use of AI-powered IoT solutions for predictive analytics, personalized treatment plans, and remote monitoring. As 5G and edge computing technologies evolve, IoT devices will become more reliable, enabling real-time decision-making and transforming healthcare delivery into a more efficient, patient-centered experience.
Have a question?
Speak to an expert








