Healthcare organizations generate nearly 30% of the world's data. However, translating this volume into timely, forward-looking decisions remains a challenge. Traditional analytics focuses on what has already happened, with limited ability to anticipate what comes next.
AI predictive analytics in healthcare helps close this gap by analyzing clinical, operational, and behavioral data to anticipate risk and support earlier intervention. Turning these insights into real-world impact, however, requires deep expertise in AI implementation in healthcare, from data integration and model reliability to secure deployment across clinical and insurance workflows.
In the article, we break down how AI-driven predictive analytics in healthcare is applied, the use cases delivering real value today, and the implementation challenges that often determine success or failure.
What is AI predictive analytics in healthcare?
AI predictive analytics in healthcare uses machine learning and statistical modeling on clinical, operational, and behavioral data to anticipate risks and outcomes before they occur. Instead of simply explaining what has already happened, it helps healthcare organizations anticipate what is likely to happen next and act before risks turn into costs or adverse outcomes.
At its core, predictive analytics gives data a "voice and a sense of foresight," enabling stakeholders to move from reactive decision-making to proactive, evidence-based strategies. AI-powered models analyze historical and real-time data, and therefore, can forecast clinical events and operational bottlenecks with a level of speed and accuracy that traditional approaches cannot achieve.
Core components of predictive analytics in healthcare
Modern predictive analytics platforms combine several foundational elements:
- Historical data to identify long-term patterns and train predictive models
- Machine Learning and AI algorithms that continuously learn from new data and refine predictions
- Real-time analytics to surface early warning signals and support timely interventions
- Integration into clinical and operational workflows, enabling clinicians and executives to understand, trust, and act on predictions
Together, these components support use cases ranging from forecasting patient deterioration and readmission risk to anticipating staffing needs and optimizing resource allocation across facilities.
How predictive analytics differs from traditional healthcare analytics
Traditional healthcare analytics are primarily descriptive and rule-based. They explain what has already happened, which works for reporting but falls short in complex clinical environments.
AI-driven predictive analytics goes further. It detects complex, non-linear patterns across thousands of variables that humans or spreadsheets would miss. For example, a slight drop in blood pressure may seem insignificant on its own, but when analyzed alongside temperature changes, lab values, and patient history, it could indicate early sepsis. Similarly, genomic data can reveal a high probability of adverse drug reactions before any symptoms appear.
The result is a shift from hindsight to foresight, enabling earlier diagnoses, more precise interventions, and better-informed strategic decisions at both the clinical and organizational levels.

By unifying these structured and unstructured data sources, predictive analytics provides a holistic view of patient and population health, supporting more personalized care, more resilient operations, and more sustainable healthcare systems.
Discover more: how generative AI can transform your healthcare operations
Predictive analytics in healthcare: Key use cases
Predictive analytics is no longer an experimental capability in healthcare but a practical tool already shaping how care is delivered, resources are allocated, and risks are managed. When powered by AI, predictive analytics enables healthcare organizations to anticipate events before they escalate, improving outcomes while controlling costs.
Below are the most impactful use cases where predictive analytics is delivering measurable value today.
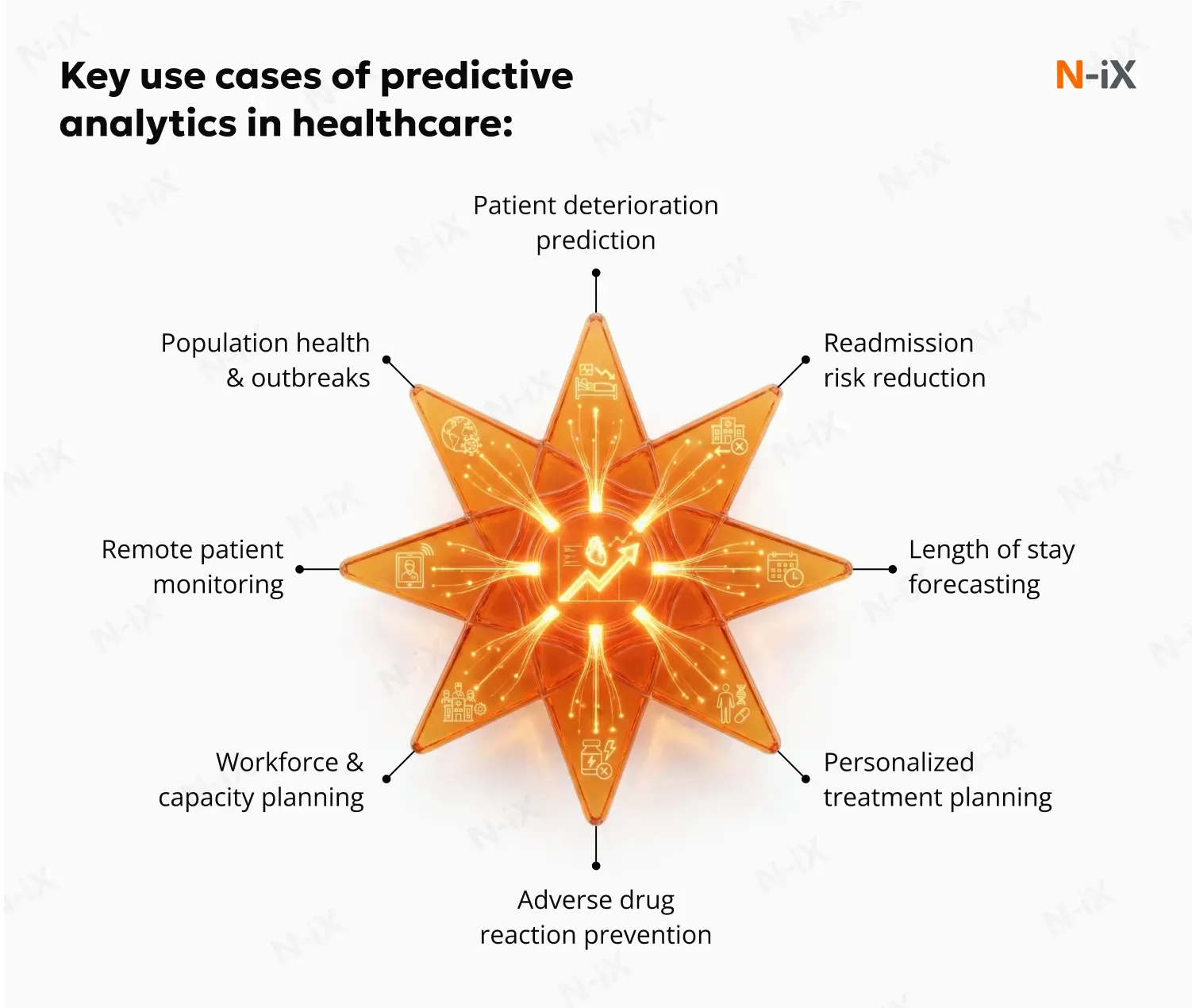
Early detection of patient deterioration and critical conditions
Hospitals use AI-driven predictive analytics to continuously analyze patient vitals, lab results, clinical notes, and EHR data in real time. These systems detect subtle, non-obvious patterns that signal deterioration, often hours or days before symptoms become clinically obvious.
Predictive models are already helping providers identify early onset of conditions such as sepsis, heart failure, acute kidney injury, and respiratory complications. Earlier alerts enable timely interventions, reduce ICU admissions, shorten length of stay, and significantly improve survival rates.
Business impact: better outcomes, lower cost of critical care, reduced strain on ICU capacity.
Reducing hospital readmissions and reimbursement risk
Hospital readmissions remain one of the most costly challenges in healthcare, affecting both clinical outcomes and financial performance. AI-powered predictive analytics helps providers identify patients at high risk of readmission by analyzing clinical history, treatment response, behavioral patterns, and social determinants of health.
Readmission risk scores are generated using clinically validated risk-scoring methods and ML techniques that evaluate medical history, utilization patterns, and social factors. These insights increasingly support predictive analytics in insurance, informing risk adjustment, reimbursement forecasting, and value-based contract performance.
Business impact: fewer readmissions, lower penalty exposure, faster reimbursements, and stronger alignment between healthcare providers and insurance stakeholders.
Predicting length of stay (LOS) and improving patient flow
AI-powered predictive models analyze historical and real-time data, including diagnoses, treatment plans, comorbidities, and operational factors, to forecast a patient's likely length of hospitalization. Accurate LOS predictions help hospitals reduce overcrowding, optimize bed turnover, minimize discharge delays, and coordinate downstream care more effectively.
Business impact: improved throughput, higher bed utilization efficiency, fewer operational bottlenecks.
Personalized medicine and treatment optimization
Predictive analytics enables precision medicine by combining medical history, genomics, imaging, lab results, and lifestyle data to tailor treatments to individual patients. AI models can recommend therapies that are more likely to be effective and less likely to cause adverse reactions. In chronic disease management, such as diabetes or cardiovascular conditions, predictive analytics supports continuous treatment adjustments based on real-time data.
Business impact: better clinical outcomes, fewer unnecessary interventions, and more efficient use of high-cost therapies.
Predicting adverse drug reactions and improving patient safety
AI-driven predictive analytics can model how specific drugs interact with a patient's genetic profile, existing medications, and physiological markers. This allows clinicians to anticipate adverse reactions before prescribing or adjust dosages proactively. Predicting drug side effects early reduces emergency visits, improves treatment adherence, and strengthens compliance with patient safety regulations.
Business impact: fewer complications, reduced liability risk, higher quality-of-care metrics.
Workforce, capacity, and resource optimization
Beyond clinical care, predictive analytics plays a critical role in hospital operations. AI models forecast patient admission peaks, bed demand, staffing needs, and equipment utilization by analyzing historical trends, seasonal patterns, and external factors.
Healthcare systems use these insights to optimize nurse and physician scheduling, reduce overtime and temporary staffing costs, and ensure critical resources are available when and where they are needed.
Business impact: lower operational costs, reduced staff burnout, improved patient experience.
Remote patient monitoring and proactive care management
Wearables and connected medical devices continuously collect patient data, including heart rate, glucose levels, oxygen saturation, and activity patterns. Predictive analytics analyzes this data in real time to detect deviations that may indicate emerging health issues. Providers can intervene earlier, often before a patient seeks care, shifting treatment from hospital-based to preventive and remote models.
Business impact: fewer hospital admissions, stronger chronic care management, scalable care delivery.
Population health management and outbreak prediction
Predictive analytics helps healthcare organizations and public health authorities identify population-wide trends and emerging risks. By analyzing clinical data alongside environmental, behavioral, and mobility data, AI models can forecast disease outbreaks and rising chronic disease burdens.
This enables earlier public health interventions, targeted screening programs, and more effective resource allocation.
Business impact: improved population outcomes, better preparedness, and reduced long-term healthcare costs.
Predictive analytics adoption: where execution breaks down
Despite widespread adoption, execution remains uneven. According to a national survey of US hospitals published in Health Affairs, 65% of hospitals use AI or predictive models, most commonly embedded into their EHR systems. However, only 61% reported evaluating these models for accuracy, and just 44% evaluated them for bias.
Implement data governance the right way—find out how!


Success!

The findings highlight a persistent gap between adoption and governance, especially among hospitals that rely on vendor-provided models and lack in-house AI expertise. Without local evaluation, predictive analytics initiatives risk producing inaccurate or biased insights that limit trust, adoption, and real-world impact.
Read more: Generative AI in healthcare: Use cases and challenges
Predictive analytics challenges and how N-iX addresses them
AI-driven predictive analytics in healthcare bring significant clinical and operational value. Yet many organizations underestimate the complexity of AI implementation in healthcare. Without the right data foundation, interoperability standards, and governance in place, even the most advanced predictive models struggle to move beyond experimentation.
Data quality, fragmentation, and interoperability
Predictive analytics models are only as reliable as the data they consume. Healthcare data is often incomplete, inconsistent, and scattered across EHRs, lab systems, imaging platforms, and unstructured clinical notes. These data silos significantly reduce model accuracy and limit real-world adoption.
N-iX solution: We build robust ETL pipelines, standardize data using FHIR, HL7, OMOP, SNOMED CT, and LOINC, and apply NLP to extract predictive signals from unstructured clinical text. Continuous data quality monitoring ensures models remain accurate as new data flows in.
Integration with legacy systems and clinical workflows
Many healthcare organizations rely on legacy EHRs and on-prem infrastructure that were not designed for real-time predictive analytics. Poor integration leads to workflow disruption, delayed alerts, and low clinician adoption.
N-iX solution: We integrate predictive analytics into existing clinical workflows using a microservices-based architecture and an API-first design. We also bridge legacy systems with modern AI components via HL7/FHIR adapters, enabling real-time predictions without forcing disruptive platform replacements. The result is actionable insights delivered directly where clinicians already work.
Algorithmic bias and fairness risks
Predictive models trained on non-representative data can produce biased outcomes, reinforcing healthcare disparities and increasing legal and ethical risks.
N-iX solution: Our engineers implement bias detection and mitigation workflows across the model lifecycle. This includes dataset audits, performance evaluation across demographic groups, reweighting strategies, and continuous fairness monitoring in production. Human-in-the-loop validation ensures models remain equitable as populations and data evolve.
Data privacy, security, and regulatory compliance
Predictive analytics requires aggregating highly sensitive health data, raising serious concerns around HIPAA, GDPR, and medical data governance. Security gaps can lead to regulatory penalties and loss of patient trust.
N-iX solution: Our team builds privacy-by-design predictive analytics architectures that include encryption at rest and in transit, role-based access controls, audit trails, and secure cloud environments. Where needed, we implement federated learning and data minimization approaches to enable model training without exposing raw patient data.
Operationalization and scaling beyond pilots
Many predictive analytics initiatives stall at the pilot stage due to insufficient MLOps maturity, inadequate monitoring, or operational complexity when models move into clinical production.
N-iX solution: N-iX operationalizes predictive analytics using production-grade MLOps pipelines. We support model versioning, performance monitoring, drift detection, and retraining strategies to ensure long-term reliability. This enables healthcare organizations to scale predictive models safely across departments and facilities.
Discover also about agentic AI in healthcare: Use cases and business value
Final thoughts
Implementing AI predictive analytics in healthcare is less about model selection and more about execution under real-world constraints: fragmented data, legacy systems, regulatory pressure, and clinical adoption. Without practical experience in these environments, such initiatives often remain limited to pilots or isolated use cases.
N-iX supports healthcare and insurance organizations in applying predictive analytics across clinical and business workflows. With 200 data and AI engineers and over 60 delivered data and AI initiatives, our teams focus on building production-ready solutions that integrate into existing systems, meet security and compliance requirements, and scale beyond experimentation. The emphasis is on reliability, governance, and measurable outcomes rather than standalone models.
Have a question?
Speak to an expert




